 “Many people with empty nose syndrome have chronic nasal dryness and infections, can’t feel airflow through the nose, have feelings of severe nasal congestion, and in worst cases, feel pain with each breath. PeopleImages/Getty Images
“Many people with empty nose syndrome have chronic nasal dryness and infections, can’t feel airflow through the nose, have feelings of severe nasal congestion, and in worst cases, feel pain with each breath. PeopleImages/Getty Images
Take a moment and inhale deeply through your nose. Feel the cool resistance in the mucous membranes as the air streams through your nostrils, warming and moistening your breath as you breathe in.
Then imagine the same nasal inhalation without that satisfying sensation of taking in oxygen. Instead, your nose feels blocked, as if you’re sucking air through a skinny cocktail straw. Or you feel you are inhaling too much air. Or the air you breathe in is too dry or too cold, making the mere act of breathing through your nose painful. These unpleasant symptoms become so unbearable that you begin to feel as if you are suffocating. You develop headaches and dizziness, become prone to nosebleeds, and sometimes wake at night gasping for air.
Yet, when you see a doctor, and he peers deep into your nasal passages, he discovers no physical cause for your symptoms. Your nose is not obstructed or deformed. Your breathing even seems OK. Perhaps, he opines, this problem is all in your head.
Or could it be empty nose syndrome?
What Is Empty Nose Syndrome?
"Empty nose syndrome is a paradoxical sense of nasal obstruction," explains Dr. Spencer C. Payne, associate professor at the University of Virginia’s department of otolaryngology. "Paradoxical because, by all measures, the nose appears really open, but the person suffering from it feels as though they can’t breathe or that air is not moving through the nose.
"And because the physics of airflow through the nose is kind of complicated, it’s hard to know if they’re truly experiencing nasal obstruction or if they’re just truly not sensing the flow of air through the nose," he says.
By some estimates, about one in 1,000 people who undergo certain types of nasal surgery develops empty nose syndrome, or ENS. There’s no telling how many people who have not undergone surgery have developed the condition. And to make matters more confusing, many doctors don’t recognize ENS as a medical condition at all.
The constant feeling of suffocating can become debilitating to those who experience it, interfering with their work, leisure activities and quality of life. Many patients reported fears they would never feel the satisfaction of a normal breath of air. With no medical professional to validate their symptoms, they become anxious and depressed.
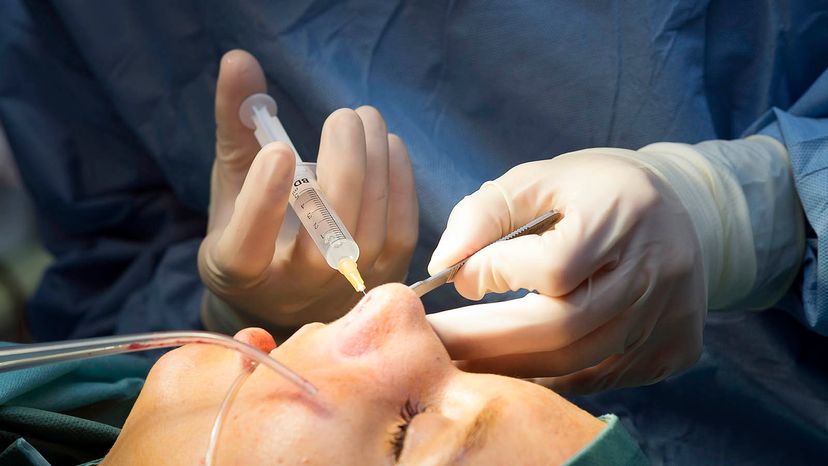 “About one in 1,000 people who undergo certain types of nasal surgeries develop empty nose syndrome. BSIP/Universal Images Group via Getty
“About one in 1,000 people who undergo certain types of nasal surgeries develop empty nose syndrome. BSIP/Universal Images Group via Getty
What Causes Empty Nose Syndrome?
It’s largely believed that empty nose syndrome is a iatrogenic condition — i.e., one caused by medical treatment — and in this case it’s nasal surgery, such as septoplasty to correct a deviated septum, cosmetic or functional rhinoplasty, or sinus surgery. During these procedures, all or some of the turbinates of the nose are removed or reduced. Turbinates are bony, mucous membrane-covered structures inside the nose, located along the sides of the nasal cavities. Turbinates regulate airflow, and warm and moisturize the air you inhale.
But even that can be a questionable cause of ENS, Payne says. Some patients who have had some or all of their turbinates removed never develop ENS. And others who have never undergone nasal surgery report symptoms of ENS.
"Although the data and research haven’t really been looked at from a total causal effect, the issue is that most patients who present with [ENS] have had surgery because they had a nasal obstruction or a sense of a blocked nose," he says. Afterward, the patient may complain that their nasal obstruction is worse than before the surgery. "So, it’s hard to know whether this failure to adequately sense airflow through the nose was triggered by the surgery or made worse by the surgery," he says.
"The truth is, we don’t completely understand why some people get it and some people don’t which is why I personally believe that it’s a combination of some underlying nerve issue that plays into it."
Is Empty Nose Syndrome Real?
In 2009, Payne was charged with writing a counterpoint to the existence of empty nose syndrome for the journal Otolaryngologic Clinics of North America. He wasn’t an expert in the field of ENS, per se. But he had studied it enough to give educational talks on the condition and had seen a few patients in his own practice with symptoms suggestive of ENS.
He dove into research, looking to side with the conventional wisdom of other otolaryngologists at the time that empty nose syndrome was more a symptom of mental disorders. Instead, he reached a far different conclusion: "The problem with empty nose syndrome is probably not that it does not exist," he wrote in the article, "it is that we cannot adequately explain its existence by what we currently understand about the nose."
Since not everyone who undergoes turbinectomy suffers from ENS, he further concluded, "it behooves us to evaluate this latter entity with a more critical eye, so that we can avoid creating future sufferers and provide relief to those who have already been afflicted."
Since then, otolaryngologists have become more open minded about empty nose syndrome, Payne says. But there are still skeptics. "There are areas of the world where they typically don’t see empty nose syndrome and it’s considered even more controversial," he says, such as Australia. He speculates that may be due to the climate.
And then there’s the anxiety and depression that often accompany an ENS diagnosis, "compounded by the sense that you’re never going to get better and no one is ever going to believe you," he says. "It would make anybody crazy.
"Depending on what side of the fence you are on, you can argue chicken or the egg," he says, adding that anxiety and depression are seen in patients with chronic disease "all the time."
Regardless, the symptoms of ENS can be so debilitating and adversely impacting on quality of life that a small number of people — especially those with underlying psychiatric problems — have been driven to suicide.
How Is Empty Nose Syndrome Diagnosed?
Diagnosing ENS is tricky as well because there are often no physical signs that can be detected during a physical examination or a scan. A diagnostic "cotton test" for ENS was developed, which involves placing cotton into a section of the nasal cavity. Researchers found the cotton to increase nasal resistance and restore airflow distribution and, for some patients, provide relief from ENS symptoms within minutes.
Some patients are assessed with the Sino-Nasal Outcome Test 22 (SNOT-22), which uses 22 symptoms to assesses nasal symptoms. More recently, a six-item questionnaire was created, called the ENS6Q, as an adjunct to the SNOT-22 test, to better identify patients with empty nose syndrome.
But those tests only skim the surface, Payne says. "There are people with empty nose syndrome in terms of a paradoxical sense of obstruction or nasal pain, and anxiety components related to it, who still have normal appearing turbinates who don’t seem to have a decrease in air flow over the turbinates. So, there’s really no great way to diagnose individuals by any objective measure other than trying to say, ‘Well, based on what the nose looks like and what you’re complaining about, then you must have empty nose syndrome.’ But, there’s no way to confirm that diagnosis."
 “Treating empty nose syndrome is difficult, but one of the most common ways is with nasal sprays, which help moisturize the nose and provide a sense of airflow. skynesher/Getty Images
“Treating empty nose syndrome is difficult, but one of the most common ways is with nasal sprays, which help moisturize the nose and provide a sense of airflow. skynesher/Getty Images
Treating Empty Nose Syndrome
Diagnosing ENS is one thing. But there are a range of treatment options for those who get a clear diagnosis. These include:
- Saline nasal sprays or gels to moisturize the nose. The evaporation of that fluid provides a sense of airflow.
- Menthol products or essential oils, like rosemary, mint and eucalyptus, to stimulate the cold receptors in the nose.
- Surgeries using implants to rebuild the turbinates or to increase nasal resistance, though these are quite rare and do not reproduce the humidification and immune protection of the original turbinate mucosa.
- Some researchers have been using platelet-rich plasma with implants to treat ENS.
- Injections of stem cells into the lining of the nose to encourage regeneration have been studied as well.
Another approach is treating not only the symptoms, but also the psycho-social distress that is a key component of empty nose syndrome. "Because you can’t cure the disease, I think it’s important to acknowledge the fact that there’s a stress and strain on the body and mind from these problems," Payne says. "And I encourage [people with ENS] to seek out psychiatric therapy just to aid in the overall treatment plan."
Now That’s Interesting
During the 2013 trial into the death of superstar singer Michael Jackson, his physician Dr. Alimorad Farshchian testified that Jackson’s insomnia — for which he was treated with a fatal dose of the anesthetic propofol and the anxiolytic lorazepam — may have been caused by empty nose syndrome. While Farshchian was merely speculating, otolaryngologist Dr. Spencer C. Payne — who did not treat Jackson — says that given the number of nasal surgeries Jackson reportedly had and how pinched his nose looked, it could be possible Jackson had ENS.














































